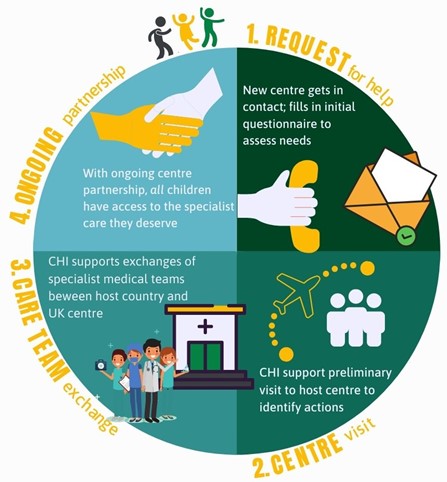
This page describes the usual methodology that Child Health International deploys to enhance the healthcare of children affected by cystic fibrosis (CF) within a particular country. However, we work collaboratively with host organisations and therefore processes may vary and evolve depending on a country’s particular needs.
We are also developing our use of virtual conferencing and electronic communications. Whilst this will likely supplement our current approach, allowing us to reach more people, the principles listed below will remain.
To find out more, or to discuss how your organisation can aid, or benefit from, CHI’s involvement, email our team at info@childhealthinternational.org.
Step 1: Request for help and preliminary questionnaire
Requests for assistance can be made by any group or individual, but typically this has been the head of a CF clinical team or parents’ association.
After initial contact is made, a member of our team will help the potential partner complete an introductory questionnaire. This helps us assess the current state of healthcare and involves collecting information on the size of the CF community, common care practices, challenges and contact details for local medical specialists or support groups relevant to our involvement.
This usually results in an invitation to arrange a fact-finding visit.
Step 2: An initial visit
The first visit usually involves the lead of a UK CF clinical team, a specialist physiotherapist or dietitian and a project manager from Child Health International. They will meet senior medical staff and representatives of a parents’ association if applicable. They typically observe in-patient and out-patient clinics and may review some difficult cases at the request of the host organisation. They may also give a lecture or demonstration to parents, patients and/or staff.
Towards the end of the visit, the clinical team will review their observations with the hosts and report back to the Board of Trustees to establish an appropriate budget and program of future support.
Each country will present its own opportunities for care improvement and this initial visit focuses on working collaboratively with all partners to identify and utilise these opportunities.
Step 3: Visits by medical teams
The key strengths of Child Health International’s approach is that it allows overseas medical staff to observe first-hand the multidisciplinary teams working within UK specialist centres, and to receive hands-on practical advice and support within their own clinics. The frequency and nature of these ongoing visits varies greatly depending on identified needs and opportunities.
Visit by UK medical team
Project teams are usually led by an experienced CF Consultant, and will include one or more of a physiotherapist, dietician and/or specialist nurse (depending on the identified needs) from one of the UK’s specialist CF centres, and a project manager. Where necessary, a competent medical interpreter may also be involved. The program may be similar to the initial visit described above or may focus on a specific skill development.
Each visit aims to develop and strengthen key relationships between relevant parties, with time set aside to refine and update project objectives and to define next steps where appropriate.
All the CF specialists Child Health International works with give their time and expertise for free, with travel expenses covered by either the charity or external funding where applicable. For example, we’ve previously received support from a host country pharmaceutical company.
Visit to UK by overseas team
Our project manager will help develop a programme of activities to ensure maximum benefit for those involved, arranging all flights, travel and accommodation for the visiting team. The project needs determine the content of the programme, which may include attending meetings, work shadowing or training in specialist areas or techniques. Early visits often give a general overview of CF case management, whilst later ones may focus on a specific activity or skill, such as lung clearance exercises, growth monitoring or diet.
Step 4: Ongoing partnership
Each project is continually assessed, refined and developed to ensure maximum benefit for the CF community in the host country. Further visits to and from the host country may involve individuals or whole teams, but will maintain a focus on developing the multi-disciplinary approach that’s fundamental to modern CF case management.
Once key relationships are established, teams can move to a more remote method of ongoing support, through email exchange or regular online meetings, requiring progressively less input from Child Health International. We aim to continue support for project teams as long as everyone agrees this is necessary, whilst ensuring that we establish partnerships that can ultimately continue independently.
Further examples of Child Health International’s activities can be found on individual project pages, or by emailing the team at info@childhealthinternational.org.




